- Community
-
Programs
- Schools
-
Careers
- RN Specialties
- Best RN Jobs and Salaries
- Aesthetic Nurse
- Nursing Informatics
- Nurse Case Manager
- NICU Nurse
- Forensic Nurse
- Labor and Delivery Nurse
- Psychiatric Nurse
- Pediatric Nurse
- Travel Nurse
- Telemetry Nurse
- Dermatology Nurse
- Nurse Practitioner
- Best NP Jobs and Salaries
- Family NP (FNP)
- Pediatric NP
- Neonatal NP
- Oncology NP
- Acute Care NP
- Aesthetic NP
- Women's Health NP
- Adult-Gerontology NP
- Orthopedic NP
- Emergency NP
- Psychiatric-Mental Health NP (PMHNP)
- APRN
- Nurse Educator
- Nurse Administrator
- Certified Nurse Midwife (CNM)
- Clinical Nurse Specialist (CNS)
- Certified Registered Nurse Anesthetist (CRNA)
- Resources
- Education

.jpg.23a321dcef651e9c4f1a9017e868ece8.jpg)
rariel
15 Posts
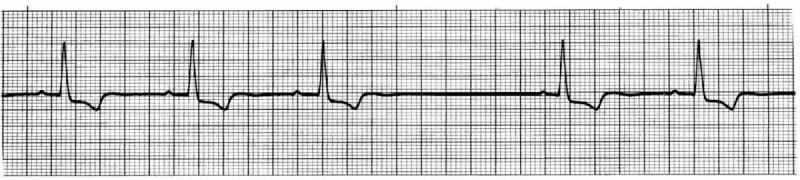
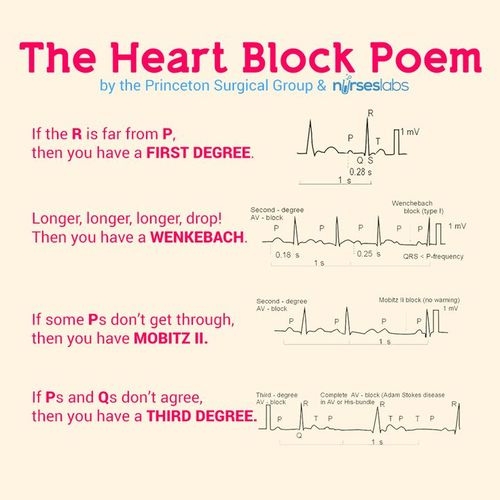
I graduated last June with my BSN and decided in December to get an advanced nursing certificate in critical care (required in Canada to work in critical care). I just finished my first clinical and there is a required ECG assignment to go along with it. I need some feedback on my answer. I want to say this is a 2nd degree AV block type I but there is no non-conducted p wave present as far as I can tell. Am I missing something here? I keep going over it again and again, but can't come up with anything. I don't need the answer but some help to point me in the right direction would be helpful.
Atrial Rhythm: _____ Regular X_Irregular
Ventricular Rhythm: ___Regular _XIrregular
Atrial Rate: 50
Ventricular Rate: 50
P Waves: present positive preceeding
PR Interval: 0.2 -> 0.24 -> 0.28 sec (then dropped beat but no non-conducted p-wave)
QRS: 0.12 sec
AV Conduction: 1:1
QT Interval: 0.4 sec
ST Segment: _____Isoelectric _____ Elevated X Depressed
T waves: _____Positive X Inverted _____Flattened ____Biphasic
Interpretation:
Anticipated Interventions: ???????